What is needed for ACA reporting?

Emma Jordan
Published Mar 03, 2026
Minimum Essential Coverage data to report For large employers, a single Form 1094-C must accompany the set of Forms 1095-C when filing with the IRS. For insurers and small employers with self-insured plans, a single Form 1094-B must accompany the set of Forms 1095-B when filing with the IRS.
Will ACA reporting be required in 2020?
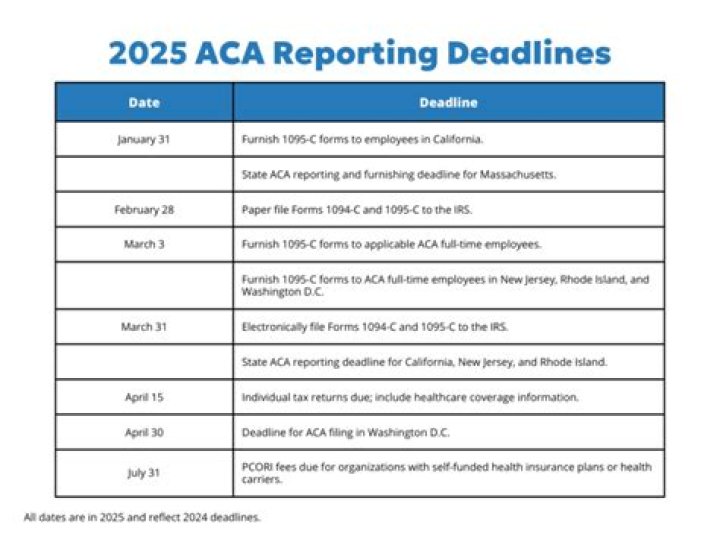
For the first time in 2021, for instance, employers who have employees who are California residents may have reporting responsibilities under California’ individual mandate, which went into effect in 2020….Deadlines Ahead as Employers Prep for ACA Reporting in 2021.
| ACA Requirement | Deadline |
|---|---|
| Electronic filing with IRS | March 31, 2021 |
Who is required to file ACA reporting forms?
All employers who offer coverage to California residents through a self-insured plan are required to submit reporting to the FTB. All self-insured employers are required to report, regardless of their Applicable Large Employer (ALE) status under the federal Affordable Care Act (ACA) rules.
Who is subject to ACA reporting?
The health care law requires the following organizations and some other parties to report that they provide health coverage to their employees: Certain employers, generally those with 50 or more full-time and full-time equivalent employees. Health insurance companies. Self-insuring employers of any size.
What is the purpose of ACA reporting?
The primary purpose of the ACA reporting requirements is to communicate certain details of health insurance coverage, including verification that the “minimum essential coverage” (MEC) is being met.
What does the ACA require of employers?
Employer mandate overview. Employers must offer health insurance that is affordable and provides minimum value to 95% of their full-time employees and their children up to the end of the month in which they turn age 26, or be subject to penalties. This is known as the employer mandate.
What are the reporting requirements for the ACA?
ACA Reporting Requirements under Section 6056 The IRS Section 6056 states that Applicable Large Employers must provide minimum essential coverage to their full-time employees and report that to the IRS and furnish statements to their employees.
What do employers need to know about the ACA?
Under the ACA employer mandate, Applicable Large Employers (ALE) must offer ICHRA to the eligible employees that are affordable and provide minimum value. Affordability for each employee is calculated based on the following criteria: For this purpose, the IRS includes the following additional fields on Form 1095-C
Who is responsible for ACA Form 1095-C reporting?
If an employee works for more than one ALEM in the Aggregated ALE Group in any calendar month, the ALEM for whom the employee worked the most hours of service in that calendar month is responsible for the employee’s Form 1095-C ACA reporting for that month.
Which is the best company to file ACA forms?
ACAwise helps to file your ACA Forms with the IRS, State and distribute the 1095 copies to your employees on-time. ACAwise handle all the special scenarios such as ICHRA, COBRA, Rehire, terminated, etc. We provide two different reporting services for you to choose from, based upon your requirements.